James was a bubbly, active little boy full of energy, always smiling, and always on the move. His mum, Yvonne, was his best friend and biggest supporter. Together, they were inseparable, spending their weekends going to the playground, meeting new people, and enjoying the little things that make early childhood so special.
“He was very social,” Yvonne recalls. “He loved making friends with other kids, with adults. He was just a really happy boy.”
So, at three years old, when James came down with what seemed like an average cold, Yvonne didn’t think much of it.
“He always got sick from childcare, so I thought this time was no different,” Yvonne recalls. “But after five days of Panadol and Nurofen, he wasn’t getting better, in fact, things were getting worse.”
Within a matter of days, James had lost the ability to walk independently.
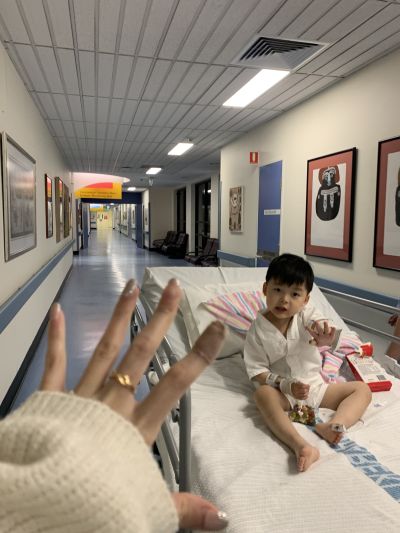
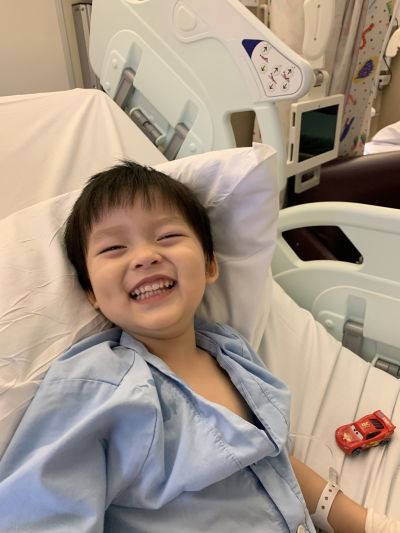
A rapid decline and a critical turning point
Desperate for answers, Yvonne saw a new GP and suddenly everything changed. This GP suggested Yvonne take James to the Emergency Department at The Children’s Hospital at Westmead, immediately.
Despite numerous tests, the cause of James’ condition remained unclear. “He couldn’t sleep, he was screaming at night, in so much pain,” Yvonne remembers. “And then we realised he was paralysed.”
Then came a turning point. Professor Russell Dale, a paediatric neurologist, was called in to examine James.
“James presented with a pretty terrifying problem,” says Professor Dale. “He had gone from being completely well to paralysed in a matter of days.”
An urgent MRI revealed spinal cord inflammation, a symptom of something much more serious. Through a cutting-edge biomarker blood test developed at the hospital, doctors diagnosed James with MOG Antibody Demyelination, a rare autoimmune condition in which the immune system attacks the brain and spinal cord.
“The biomarker test was critical,” Professor Dale explains. “It told us exactly what was wrong and, more importantly, how to treat it. Without it, James could have faced a lifetime of disability.”
World-leading treatment that changed everything
Treatment began immediately. High-dose steroids were administered to reduce the inflammation, and within days, James began to regain movement in his legs.
“I was shocked,” Yvonne says. “He went from not being able to move at all to starting to kick his legs in bed.”
But just weeks later, as they thought they were through the worst, James suffered a second attack, this time affecting his vision.
James underwent monthly IVIG treatments and weekly physiotherapy for six months. He missed time at childcare, and Yvonne, who had already deferred her final university exams, juggled it all alone.
“I didn’t have family here, but at the hospital, the social workers, the doctors, the nurses, they were all so kind. I’m so grateful for the care we received.”


Rebuilding strength and rediscovering joy
James spent months recovering and rebuilding. And today? He’s back to being the bright, curious, happy little boy he was before.
“He plays violin now, we play together,” Yvonne smiles. “And he loves tennis and drawing. He’s just a happy kid.”
The decision to introduce James to music was inspired by a volunteer who visited the hospital ward.
“She came in playing guitar and singing to the kids, and I remember thinking how beautiful it was, how much joy she brought,” Yvonne says. “Maybe one day James can do that for someone else.”

Why your support matters for kids like James
James is living proof of what’s possible when clinicians, researchers and supporters come together. But these discoveries don’t fund themselves, they happen because generous people choose to make a difference.
Yvonne knows exactly what that difference looks like: a little boy who can walk, laugh, and play again.
You can be part of what’s next. Donate to Sydney Children’s Hospitals Foundation today to change the future for kids like James.












